Frequently Asked Questions
What is the US Family Health Plan?
The six US Family Health Plans are among the health care choices for eligible beneficiaries under the Department of Defense’s TRICARE Prime program. Health care is provided to active duty family members, activated National Guard and Reserve family members, and retirees and their family members. Care is provided through six large regional civilian health care networks of primary care physicians, hospitals, and affiliated specialists.
The US Family Health Plans offer an outstanding program of health care and wellness management built on a foundation of leading-edge health care techniques, wellness rather than disease management, an understanding of what it means to be a member of the military family, and unsurpassed commitment to our members.
Is US Family Health Plan separate from TRICARE or part of TRICARE?
US Family Health Plan is one option of the Military Health System known as TRICARE. The US Family Health Plan program was selected by the Department of Defense to be a provider of TRICARE Prime. As a US Family Health Plan member you receive all the benefits offered by the TRICARE Prime program. The US Family Health Plan has served the health care needs of military beneficiaries since 1993.
However, the US Family Health Plan providers began as US Public Health Service hospitals. The Department of Defense has contracted with the former US Public Health Service hospitals and their successors since 1982, and the current TRICARE Prime contracts under which the US Family Health Plan is now operated are a continuation of this long standing partnership relationship under which eligible beneficiaries receive healthcare.
Who is eligible to enroll in the US Family Health Plan?
Any beneficiary under the age of 65 who relies on the Military Health System for their health care and who is eligible in the Defense Eligibility and Reporting System (DEERS) is eligible to enroll in the US Family Health Plan. The DEERS list includes anyone who is eligible to receive military health benefits, including active duty family members, retirees, retiree family members, and activated members of the National Guard and Reserve.
Active duty personnel are not eligible; they are required to obtain their health care at Military Treatment Facilities (MTFs) or through another TRICARE program.
Why should I choose the US Family Health Plan for my health care?
US Family Health Plan offers military families and retirees patient-centered health care with the highest satisfaction level in the TRICARE system. Members have access to advanced medical care and services in the communities in which they live. Our providers have a deep understanding of military culture and of the unique components of care associated with the military community.
May we use a military treatment facility while enrolled in US Family Health Plan?
Not for routine or urgent care. Under the US Family Health Plan, you may not use military treatment facilities. The only exceptions to this limitation are if you have an acute medical emergency and the military treatment facility is closest to you, or if there is an agreement between the US Family Health Plan and a military treatment facility that allows US Family Health Plan enrollees to be referred to the MTF for specialty care.
Are prescriptions covered under US Family Health Plan?
On January 1, 2022 changes in pharmacy copays for military health plans took effect.
Please note: Pharmacy copay changes do not affect dependent survivors of active duty service members. They also do not affect medically retired service members and their dependents.
These changes are required by law and affect TRICARE beneficiaries. The new copays are listed in the chart below:
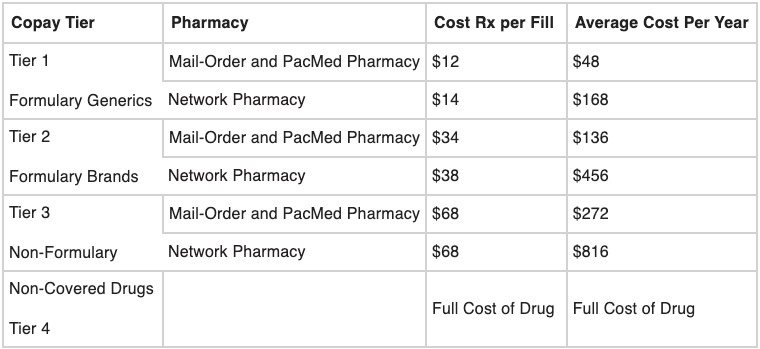
Source: www.tricare.mil/Costs
What if we move?
If you move within your current Plan’s zip code-defined service area, simply notify the Plan of your new address. If you want to change your primary care provider to accommodate your new address, there’s no problem. Give us a call and we’ll send you a new membership card with your new PCP’s name and phone number.
If you move to one of the other areas across the country where the US Family Health Plan is available, we will be happy to transfer your enrollment for you.
If you move to an area where the US Family Health Plan is not available, we can give you the information you need to transfer your enrollment to the regional TRICARE Prime program.
What if I unexpectedly become ill when I’m on vacation?
The US Family Health Plan covers you for medical emergencies wherever you are. Go to the nearest appropriate medical facility and please be sure that someone calls the Plan (either the 800 number or your primary care provider’s phone number) within 24 hours, so your provider can confer with the attending doctor. Your costs will be covered for everything above your copayment. Show your US Family Health Plan membership ID card and have the bill sent to the address on the back. Plan members may use Military Treatment Facilities for medical emergencies if the MTF is the nearest emergency facility to you when you become ill or injured.
When can I enroll in US Family Health Plan?
Enrollment is open all year to enrolled PRIME beneficiaries. TRICARE Select beneficiaries are limited to enroll during open season; unless there is a qualifying life event during the year.
May I participate in the US Family Health Plan if I am 65 years or older?
That depends on when you enrolled in the US Family Health Plan.
If you enrolled in the plan on or before Sept. 30, 2012, and have remained enrolled, you may receive your care through the US Family Health Plan even after you turn 65.
If you enrolled in US Family Health Plan on or after Oct. 1, 2012, the law requires that you be transferred to Tricare For Life when you turn 65.
Where is the US Family Health Plan available?
The US Family Health Plan is available in the District of Columbia and 16 states. If you live in New England, the Mid-Atlantic, the Western Gulf Coast or in the Puget Sound area you may be eligible for the plan. Each of the six designated provider organizations under the US Family Health Plan provides care to eligible beneficiaries in a geographic region based upon zip codes. In brief, the designated provider organizations and their service areas are as follows:
-
- US Family Health Plan of Southern New England (Brighton Marine)—Serving Massachusetts, Rhode Island, parts of Southern New Hampshire and Northern Connecticut
-
- Christus Health—Serving Houston, TX San Antonio, TX Leesville, LA and Lake Charles, LA
-
- Martin’s Point Health Care—Serving Maine, New Hampshire, Vermont, Upstate and Western New York and parts of Pennsylvania
-
- Pacific Medical Center—Serving Western Washington, most of Central and Eastern Washington, Northern Idaho, Western Oregon, and most of California
-
- USFHP@SVCMC,Inc—Serving New Jersey, Western CT, Lower Hudson Valley, NYC including Nassau and Suffolk counties, and Pennsylvania.
